REDPOINT FOR PAYERS
Power Member Engagement and Activation With a Foundation of Trusted Data
Go beyond clinical data to build the most complete member profiles — driving better health, higher satisfaction, and lower costs.

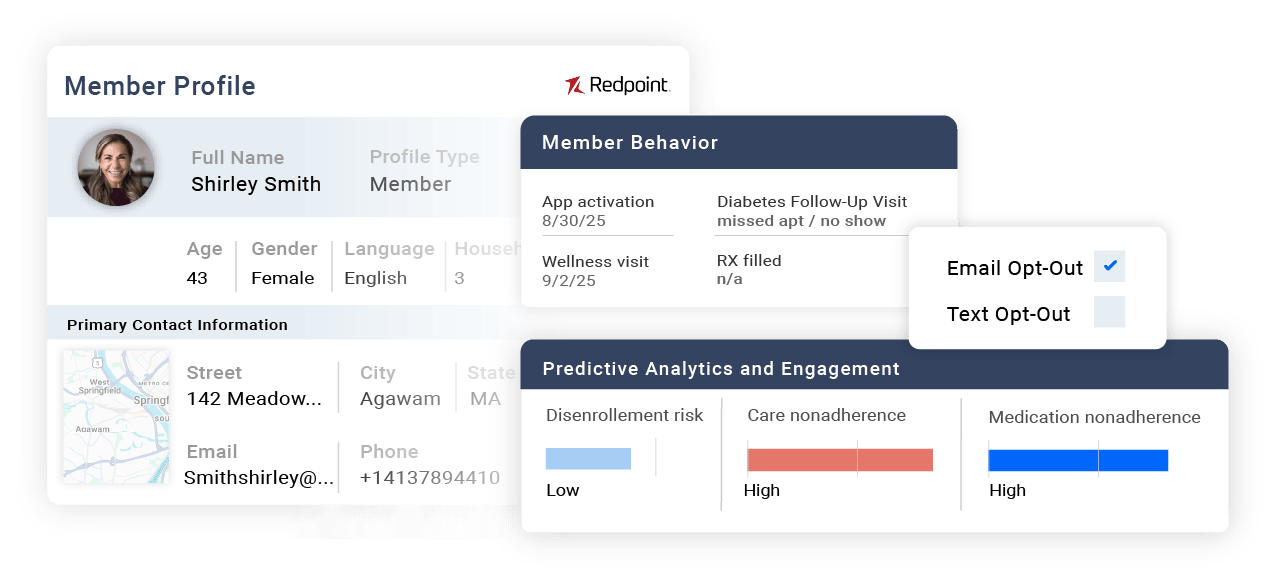
Your member data is everywhere.
Your view of the member shouldn’t be.
Fragmented systems, complex data sets and hard-to-resolve identities make it difficult to understand or meaningfully engage members. Redpoint unifies clinical, claims and consumer data into a single, accurate, real-time member profile.
Guide Every Member to Better Outcomes

Understand Complete Member Context
Connect and orchestrate data from every source at enterprise scale. Redpoint links complex identities, transactions, behaviors and data models, delivering the context and clarity you need to personalize with confidence.

Identify the Right Members for Your Programs
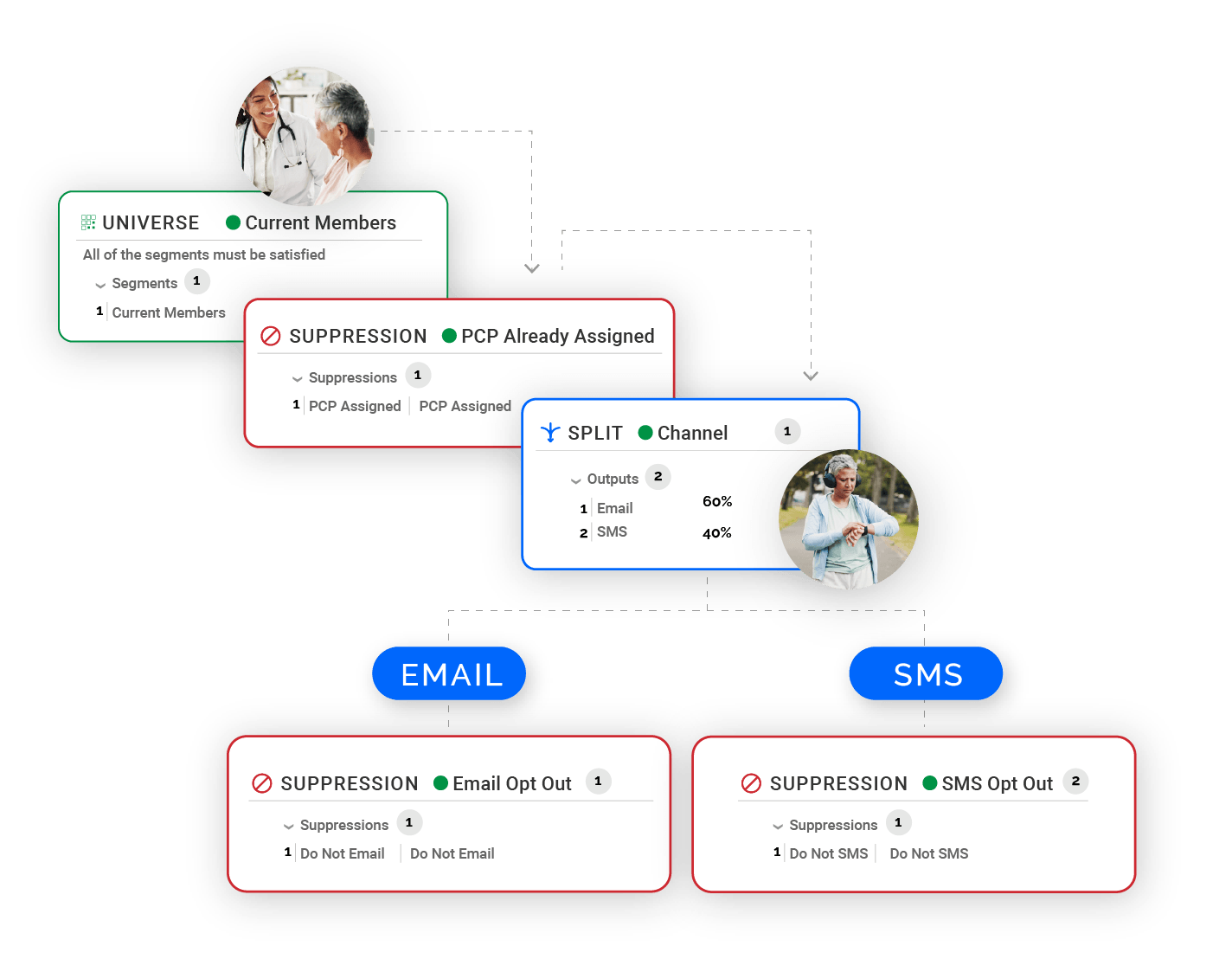
Use one trusted hub to pinpoint the right members and guide them to the right care through personalized omnichannel communication driven by data, insights and dynamic feedback – seamlessly coordinated to prevent friction.

Predict & Trigger the Next-Best Action in Milliseconds
Respond to members’ needs the moment they arise. Redpoint listens for real-time, event-driven signals to trigger the next-best action across channels, proactively guiding members through their care journey.
Fuel AI & Analytics with Trusted, Cleansed Data
Improve model accuracy, sharpen risk targeting and strengthen value-based care performance with clean, unified member profiles. Accelerate care gap identification and support risk adjustment with data your AI models can trust.
Proven Impact
Payers using Redpoint report measurable improvements across engagement and operations:
Higher Engagement
50% more
appointments scheduled
Smarter Spend
20% lower
marketing cost
Faster Activation
80% reduced
data prep time
We wanted to help members navigate their benefits effectively, enabling them to gain the maximum value from their plan. We began prompting them with real-time recommendations, all driven by the Redpoint platform. When a member logs in, we deliver the most relevant recommendations based on where they are in their journey, ensuring they maximize the value of their plan.
– EXECUTIVE DIRECTOR, DIGITAL ENGINEERING AND TRANSFORMATION
How Payers Use Redpoint for Data Readiness
Activate trusted member data to improve quality performance, manage cost, ensure compliance, and deliver better experiences across the payer ecosystem.
Quality, Stars & Value-Based Case
- Care Gap Closure
Identify and prioritize members with open care gaps and activate timely, personalized outreach to improve quality measures, Star ratings, and health outcomes. - Pre-CAHPS Program
Use integrated survey, engagement, and member data to proactively improve CAHPS outcomes through targeted pre- and post-survey interventions. Learn more - Annual Wellness Visit
Activate eligible members to complete AWVs, supporting accurate risk adjustment, improved quality scores, and proactive care planning. Learn more - Medication Management & Adherence
Enable targeted medication reviews and adherence programs to improve outcomes, enhance Part D Star Ratings, and reduce avoidable medical spend. - Chronic Care Management
Support ongoing therapy compliance and care coordination using unified clinical, claims, and engagement data to improve quality incentives and member quality of life.
Total Medical Spend
- Care Program Enrollment
Ensure the right members are enrolled in the right care management programs by using trusted, timely data to drive precision targeting and activation. - Prevention & Wellness Programs
Increase enrollment and sustained engagement in prevention and wellness initiatives to reduce long-term medical costs and improve population health. - Accurate Risk Adjustment
Support appropriate documentation and member actions, such as health risk assessments, to ensure accurate risk scores and fair reimbursement.
Member Experience & Growth
- Welcome & Onboarding
Deliver personalized onboarding experiences that help new and returning members understand benefits, access care, and engage early. - AEP/OEP Lead Generation
Identify and engage high-propensity prospects across channels using trusted data to improve conversion and lower acquisition costs. - Medicare Age-In
Identity and nurture commercial members approaching Medicare eligibility with timely, relevant education and engagement. - Digital Adoption (Portal & App)
Drive adoption of digital self-service channels to improve member experience while reducing administrative costs. - NPS & Satisfaction Surveys
Orchestrate survey outreach and follow-up actions using integrated member data to continuously improve satisfaction and loyalty.
Provider Network Performance
- Directory Accuracy & Compliance
Maintain accurate, compliant provider directories by continuously reconciling provider data across internal and external sources. - Provider Network Management
Unify provider, claims, quality, and engagement data to support accurate directories, proactive provider outreach, and stronger relationships across the network. - Provider Engagement & Enablement
Support targeted provider communications (quality initiatives, value-based programs, administrative updates) using clean, current data to reduce friction and improve collaboration.
Equitable, Whole Person Care
- Behavioral Health Engagement
Integrate physical and behavioral health data to identify unmet needs and connect members with appropriate behavioral health programs. - Health Equity & SDOH
Layer clinical, claims, and social determinants data to identify care disparities and connect members with community resources such as housing, nutrition, or transportation support.
Uncompromised Data Security
Data readiness means never compromising data security. With Redpoint, secure data behind your firewall, use your data cloud, or entrust it to us. Redpoint seamlessly adapts to your organization's security requirements.
Enterprise-grade Security and Compliance










